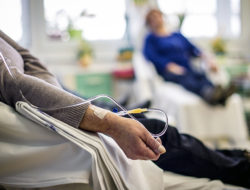
A new acronym has crept into the lexicon: CRISPR, which stands for “clustered regularly interspaced short palindromic repeats.” It’s a naturally occuring string of bacterial genetic code, and when it’s combined with the enzyme Cas9, it becomes a groundbreaking scientific tool that can precisely edit a genome, homing in on genes of interest, removing them, and even replacing them with different ones.
The CRISPR-Cas9 technique—usually just CRISPR for short—has become a go-to laboratory staple because it’s easier to use than previous gene editing techniques and produces good results. That’s not to say it’s perfect. There are still concerns about accidentally editing the wrong genes, producing off-target effects.
There are also ethical questions. Recently, researchers edited a disease-related gene in human embryos, sparking both excitement and soul-searching. Is this the first step toward designer humans?
If so, that won’t be for a long time. Meanwhile, CRISPR is changing how lab research is done, accelerating scientists’ ability to answer profound questions about biology. In the next few years, we could start seeing CRISPR products in hospitals, farms, and even gas stations. CRISPR is about to change our lives.
Your CRISPR Primer
CRISPR is not the first gene editing technique—and it won’t be the last—but for now it is the easiest to use. The approach is having a dramatic impact on bench research and product development and will ultimately change patient care.
Other editing techniques like zinc finger nucleases and TALEN work, but generally aren’t as versatile, precise, or user-friendly as CRISPR. This ease of use is a big deal. It’s kind of like the moment, 30 years ago, when the world went from DOS computers to Windows. Suddenly, everyone could use a PC.
“CRISPR opened gene editing to the masses,” says Eric Ostertag, CEO at San Diego–based Poseida Therapeutics. “It was easy to design, easy to create. You didn’t need a lot of knowhow.”
Like so many scientific techniques, it was borrowed from nature. Bacteria store the DNA of viruses they’ve encountered before in CRISPR strings for future reference, like antibodies in an immune system. The next time that particular virus attacks, CRISPR “recognizes” the target DNA and Cas9 homes in and cuts it out, stopping the virus from reproducing.
“Is this the first step toward designer humans?”
Sometimes this gene removal is all that researchers need to make use of. They often cut out genes to investigate their function. (“What happens when you take this one away?”) Other times, scientists add a replacement gene, perhaps to correct a disease-causing mutation.
Because the CRISPR technique is relatively fast and easy, it can edit multiple genes at once. This can be incredibly useful, especially when studying a complex disease such as schizophrenia, in which many genes may be involved. In 2015, researchers in Harvard’s Church Lab made 60 gene edits at once. This breakthrough led to a Boston company called eGenesis, which is using CRISPR to make pig organs safe for transplant.
In the scientific community, CRISPR dominates conferences and journals and has dramatically accelerated research. It has rapidly become an essential laboratory tool.
“This has dramatically changed work in the lab on so many levels,” says Jun Wu, a staff scientist in the Izpisua Belmonte Lab at the Salk Institute. “With this tool, we can target, do gene knockouts, disable genes, introduce genes.”
The Places We’ll Go
While editing human embryos garners lots of headlines, CRISPR is having an even greater impact in animal studies. Researchers at Sanford Burnham Prebys Medical Discovery Institute and Stanford University recently used CRISPR to knock out four Id family genes in mice. These genes proved crucial for heart development. Without them, no hearts developed at all. The work could ultimately help scientists and clinicians produce large numbers of cardiac progenitor cells—more mature stem cells that could help treat cardiovascular disease.

This was the first time all four Id genes had been knocked out. The previous record was three, which had been accomplished only with some difficulty. Prior to CRISPR, it might have taken two or three years to take out a single gene. For this study, the team knocked out four genes in 18 months. CRISPR made the work possible.
“Simply numerically, it was impossible to do,” says Mark Mercola, professor of medicine at Stanford and adjunct professor at SBP. “A triple knockout was a true tour de force ten years ago.”
While the system needs refinement before moving into the clinic, CRISPR technologies could really help patients. Combined with sophisticated delivery systems, gene editing could be used to correct somatic cells (i.e., those that aren’t part of the reproductive process, like nerve or muscle cells).
“Germline editing catches a lot of attention nowadays,” Wu says, “but CRISPR is also powerful for somatic mutations.”
CRISPR’s ability to accelerate basic research is also driving product development, and the applications are legion.
“This is a very important research tool,” says Todd Peterson, chief technology officer at La Jolla–based Synthetic Genomics. “It’s extremely useful for basic research, and there’s a growing list of applications, from clinical indications to improving food, improving fuels.”
Synthetic Genomics is in the business of manipulating DNA to develop pharmaceuticals, vaccines, and other products, so gene editing has been a godsend. In some cases, CRISPR is like using a word processing program instead of a typewriter. With the latter, big mistakes cause a typist to start from scratch. With a word processor, those same mistakes can simply be overwritten.
“It makes it easier in very large DNA molecules to go in and cut out the region you want to change,” Peterson says. “Before, you would have to resynthesize the entire large piece at considerable cost and time.”
One realm where this cost-saving can be put to use is in CAR-T immunotherapy, which treats B-cell acute lymphoblastic leukemia. Kymriah, a CAR-T therapy by Swiss company Novartis, can be incredibly effective, but it’s also $475,000 and cumbersome to use. It must be completely personalized: Each patient’s T-cells are drawn and modified to make them cancer-fighting machines, then reinfused into the patient.
Poseida Therapeutics, a San Diego company, is developing an off-the-shelf CAR-T that uses CRISPR to do that modification, resulting in a product that could, in theory, be given to anyone.
CRISPR’s Ethical Yin and Yang
Every once in a while, a research paper explodes. That’s what happened with “Correction of a pathogenic gene mutation in human embryos,” which was published in Nature a few months ago.
Jun Wu and other Salk colleagues, along with researchers from Oregon Health & Science University and other groups, targeted a mutated gene (MYBPC3), which raises the risk of cardiovascular disease and sudden cardiac death, and repaired it in human embryos.
The embryos were never implanted—that would be illegal in the United States—but this proof of concept sent shock waves through the scientific community and inspired more than a few scary headlines.
Germline editing (altering the genes that are passed on from one generation to another) is the stuff of dystopian science fiction. If we start editing human germlines, where do we stop?
“Potentially, it’s a zero-sum game. We don’t fully understand these things.”
“Most people would be very uncomfortable with choices that would somehow enhance an individual,” says Michael Kalichman, founding director of the UC San Diego Research Ethics Program. “For example, this collection of genes will help them run faster or be smarter or taller.”
On the other hand, gene editing could eliminate some dreadful diseases: cystic fibrosis, sickle cell, Huntington’s disease. The Oregon and Salk researchers proved it’s possible. But even these focused interventions have gray areas.
“What if someone identified a gene involved in deafness?” Kalichman asks. “It’s not necessarily a disadvantage, just part of a certain culture. I would prefer to err on the side of not doing these things until society has given it enough thought.”
The ethical questions pile up fast. If legalized, these techniques would be quite expensive, which could further stratify society. There’s also the possibility of off-target effects. What happens if, in the process of correcting a disease gene, clinicians create a new mutation that is passed on to future generations?
There aren’t many mutations guaranteed to cause disease. Mostly, genomic variations adjust the probabilities: mutation X will increase the risk of developing condition Y by 35 percent. In some cases, disease-causing mutations can offer health benefits. People with sickle cell are resistant to malaria, though it’s generally not a good trade.
“Potentially, it’s a zero-sum game,” says Kalichman. “We may not know the implications of adding a gene or taking it away—how it interacts, how it functions. We don’t fully understand these things.”
For Kalichman and other ethicists, these possibilities don’t inspire fear but rather a calm, ongoing consideration. A recent paper by the American Society of Human Genetics summarized the potential risks and benefits of germline editing.
The ASHG paper notes that, even if the technique works, it still changes genomes for future generations without their consent. In addition, if all “errors” can be fixed, how might that affect unconditional parental love? Could it inspire a eugenics revival, despite the ugly history?
The paper concludes that it would be “inappropriate to perform germline gene editing that culminates in human pregnancy.” Still, the authors feel the research should continue, particularly in nations that have robust regulatory systems to monitor these efforts, like the United States.
“It’s a box full of thousands of different shiny objects,” Kalichman says. “What you apply the technology to generates very specific questions about what it means to change a species—whether it’s a plant or an animal or a fungus or humans. We are at the beginning of an extraordinarily promising technology. Because it’s new, there are also an extraordinary number of unknowns that we will be facing. We all need to be involved in figuring out what that means as we move forward.”
Who’s using CRISPR?
Given the technique’s immense power and popularity, it might be easier to ask: Who’s not using CRISPR? However, we wanted to give a small sampling of the many applications at work in San Diego labs. Apologies to those we miss.
UC San Diego scientists have jumped on CRISPR in a big way. One group used a modified CRISPR technique to target RNA and repair defects associated with Huntington’s disease. Another team edited genes associated with retinitis pigmentosa. Others used CRISPR to identify 120 potential targets for cancer drugs. By knocking out the genes, they could determine their function and show how their loss affects tumors.
Scientists at the Scripps Research Institute have used CRISPR to activate HIV from hibernation, potentially making it easier to eliminate the virus with current therapies.
Researchers at Salk and Oregon Health & Science University edited out a gene in human embryos associated with heart disease. This proof of concept could eventually lead to techniques that could eradicate certain inherited diseases.
Researchers at Synthetic Genomics and Exxon Mobil have used gene editing to double fuel yields from algae, which could make biofuels more economically feasible.
Other San Diego companies working with CRISPR
- Agribody Technologies
- Allele Biotechnology
- Arcturus
- CureMatch
- Genomatica
- Poseida
- Solstice Biologics
- Synthorx